| |
Colonial Medicine
Australia's First Doctor
The first European doctor to set foot in Australia was Frans Jansz, who was the ship's surgeon on the Dutch ship Batavia. He came also with his assistant surgeon Aris Jansz. Their ship was the pride of the Dutch East India Company and was on its maiden voyage when it was shipwrecked on Houtman Abrolhos in 1629 (about 40km west of the area now known as Geraldton). Amongst the 220 survivors was another medical practitioner, Jeronimus Cornelisz, an apothecary. He took charge of the survivors whilst the ship's commander, Francisco Pelsaert, sailed in a longboat to the east to the Western Australian coast. Here he sought to find water, but having found none, proceeded to sail north to Jakarta, where he was supplied with a rescue ship. In the 15 weeks that Pelsaert was away, Cornelisz organised a band of mutineers who brutally murdered all but 80 of the survivors, including most of the children and women. The executions and rapes that occured make it the worst page in Australian history. Frans Jansz was amongst the many who were murdered by Cornelisz's mutineers.
The Convict Era
The First Fleet
The First Fleet consisted of 11 ships that left
Great Britain on 13th May 1787 to arive in Botany Bay in 18th January
1788, having sailed 251 days. The fleet consisted of two Royal Navy
vessels, three store ships and six convict transports, carrying more
than 1,000 convicts, marines and seamen. It had stops in Santa Cruz at
Tenerife, Rio de Janeiro and Cape Town. This was one of the world's
greatest sea voyage, 1,487 people in total traveling 24,000 km. There
were 48 deaths on the journey (~3%). There were 10 doctors on the 11
ships. The diary of Mr Arthur Bowes Smyth (who was one of the 10) still exists and gives a good account of life on the voyage. The doctors had to deal with all the medical problems for the
journey. The following stayed in Australia to support the new colony;
- Assistant Surgeons
- Balmain
- Arndell
- Considen
- John Irving
Over the total peiod of transportation, about 350 doctors mage the
voyage to Australia (and back for many). Some more than once. Also, 112
doctors arrived as convicts (of the 160,000 people transported as
convicts)7
The Second Fleet
Medically the second fleet was a disaster compared to the first.
The contracted shipping company was paid for every convict accepted, not
delivered. in fact there was a perverse incentive to have the convicts
die along the way.. it meant that they could also sell the provisions
not needed. Of the 939 male convicts and 78 females embarked, and only
692 males and 67 females landed at Port Jackson. This meant that 759
convicts arrived alive. of these 500 were sick and/or dying. The second
fleet brought with it a portable military hospital. The medical sevices
were overwhelmed.
|
 Courtesy of Mitchell Library
Courtesy of Mitchell Library |
Some Early Doctors
First doctors in the colony were the ships' surgeons (in the navy or
army) but were not always qualified. Over time, more doctors came, many
earning their passage by working as the ship doctor. There was little
scope for private practice in the early days medical services were
provided by the Colonial Medical Service. It initially consisted of five
doctors for the colony. They were to primarily treat the military and
the convicts. They were employed directly by the government (British
Treasury) and worked in tents. There were very few free settlers at this
time. Population health (quarantine and smallpox vaccination) was
organised by the various governors.
1788 - John White (1750 - 1832) was the principal surgeon for the first
fleet. He had served as a surgeon's third mate from 1778 and was
promoted to surgeon in 1780. In 1787 he joined the First Fleet at
Plymouth and traveled to the new colony of NSW on the Charlotte.
In 1788 he was appointed as Surgeon General for NSW. Within a week of
the arrival in Port Jackson, he and his team had to deal with scurvy and
an outbreak of dysentry. The lack of medical supplies encouraged him to
explore the native flora as a source and in 1788 was distilling
eucalyptus oil. He wrote A Journal of a Voyage to New South Wales (1790), in which he described many Australian species for the first time. White disliked Australia and returned to England in 1794.
1788 - Arthur Bowes Smyth (1750-1790), surgeon, was born on 23 August 1750 at Tolleshunt. He served on the Lady Penrhyn. His voyage was recorded in great detail in his diary, Journal of Arthur Bowes Smyth, 1787 March 22-1789 which is a rich source of information on the life aboard one of these convict ships.
|
1790 - D'Arcy Wentworth (1762-1827) came voluntarily to Botany Bay in 1790 on the second fleet ship, the Neptune
as the assistant surgeon. Having been born in Northern Ireland, he
attended medical school in London. He was accused of highway robbery,
and although he was not found guilty, he was advised to leave. Upon
arrival he worked for four years at Norfolk Island. He then moved to
Sydney, where Governor Lachlan Macquarie made him Chief of Police and
Treasurer of the Police Fund. From 1809 - 1817 he was the Principal
Surgeon. Wentworth gained considerable wealth from the contract to build
the Sydney Hospital. The contract gave the sole rights to import rum to
the colony. Consequently the hospital was called the Rum Hospital.
|
 |
"As a medical practitioner, Mr. Wentworth was distinguished for the
tenderness with which he treated his patients of every degree, and
especially that class of unfortunate persons whom the charge of the
General Hospital placed so extensively under his care. He was peculiarly
skilful in treating the diseases of children"9.
He became a founding director and major shareholder of the Bank of NSW. Wentworth died at his property Homebush
in 1827. The Sydney suburbs Homebush and Wentworthville derive their
names from his property and his name. His son, WC Wentworth, became
famous for his exploration and his work as a colonial lawyer, helping to
shape the early laws of Australia.
 |
1801 - William Redfern (1774 - 1833) was sentenced to death for mutiny,
but his sentence was commuted to life imprisonment. He had trained as a
surgeon's apprentice under his older brother and passed the
examinations of the London Company of Surgeons in 1797. He became a
surgeon's mate in the navy. He was transported in 1801 after four years
in gaol was and given a conditional pardon on arrival in Sydney. He was
transferred to work on Norfolk Island as an assistant surgeon. Although
he received a full pardon in 1803 he remained until 1808 at which time
he was appointed as an assistant surgeon at the new Sydney Hospital. He
resigned from the Colonial Medical Service in 1819 and developed a large
private practice. He became a founding member of the Bank of NSW. The
suburb of Redfern is named after him. Further information here.
|
1813 - The first Australian medical student, James Shears was
apprenticed to William Redfern. Following his death a year later, Henry
Cowper, aged 14, took his place. Medical training in the early colonial
period, usually consisted of apprenticeship to a doctor followed by
going to England for further training and examinations.
1814 - Dr William Bland arrived in Australia. He was sentenced to seven
years transportation for killing a ships purser in a dual, whilst
working as a naval surgeon. He was assigned to work in the Castle Hill
Lunatic Assylum. Pardoned a year later, he set up as the first
Australian doctor in full-time private practice.
1815 - In England, the Apothecaries' Act of 1815 was passed. This gave
the Society of Apothecaries the right to hold examinations and grant
licences to practice medicne. At this point in time in England there
were three groups of medical practitioners:
- physicians
- surgeons
- apothecaries (who became, over time, general practitioners!)
Membership of the Society of Apothecaries, at this time, required a
five year apprenticeship and then a viva voce examination (to which,
later, a written examination was added).
However, there were numerous other groups vying to treat the sick and
injured. These included barbers, quacks, druggists, chemists,
unqualified persons and vendors of empirical remedies. The druggists and
chemists eventually formulated their own body and became the
Pharmaceutical Society of Great Btitain.
1827 - The Sydney Dispensary is set up to provide outpatient care to the
poor. It is financed by charitable subscriptions and donations. It
later became the first public hospital in Australia: Sydney Hospital.
The Later Colonial Era
Note that doctors in this era often had considerable interests outside of medicine, including political careers and farming.
The 1830s
1831 - the first friendly society was set up by boat builders to provide health insurance.
1832 - The British Medical Association was founded in England
1835 - The government subsidised the Sydney Dispensary on a pound for pund basis.
1838 - The NSW Medical Board was formed via an act of parliament (2 Vic., Act No. XXII): 'An
Act to define the qualifications of Medical Witnesses at Coroner's
Inquests and Inquiries held before Justices of the Peace in the Colony
of New South Wales'. The Act states that:
- A coroner or justice of the peace (JP) can call upon the nearest
practicing, registered medical practitioner to attend a coroner's
inquest or JP's inquiry.
- For this to happen, there had to be a register of qualified practioners.
- Those to be admitted would be those doctors who had either:
- a Bachelor of Medicine of some university or
- a physician or surgeon licensed by or admitted into a college of physicians or surgeons in Great Britain or
- a member of the Comany of Apothecaries in London or
- a Medical Officer "duly appointed and confirmed by Her Majesty's sea or land service".
- The Governor may appoint a board of not fewer than three
members of the medical profession to be the NSW Medical Board. They
shall examine the qualifications of the applicants to the medical
register
- The Medical Board of NSW shall keep a written register of the qualified medical professionals.
1839 - The Deputy Inspector General of Hospitals intoduced a new system
of medical administration. The Colonial Surgeons submit their
resignations in protest. These are not accepted so as to avoid paying
retirement allowances.
The 1840s
The running of convict hospitals was given to local trustees. Doctors
worked in an honorary position. Few hospitals charged fees. Many small
privately owned hospitals started to appear, funded by subscriptions and
government subsidies.
1842 - The Medical Register was commenced in Victoria in Port Phillip.
1844 - The Medico-Chirurgical Association of Australia was formed by Dr William Bland and colleagues.
1846 - Port Phillip Medical Association (PPMA) was formed by 12 doctors.
The objectives were to develop a code of ethics, meet to discuss
scientific papers, set up a library and publish a journal. The
formulation of the code of ethics was divisive. The journal was
published but lasted only 6 were handed over to hospital boards for management. They are no longer under military control.
1847 - The first general anaesthetics were given in Australia. Ether had been used as a recreational drug in America in the 1700s and 1800s, particularly by academics at "ether frolics". The first known use for medical purposes was probably by a medical student, William Clarke, who administered it for a dental extraction in January 1842. A rural physican, Crawford W. Long, used it in his practice in Jefferson, Georgia from 1842 onwards, but did not report its usage until much later.
| The first demonstration of ether as a general anaestheic was given in America by a medical student/dentist, William Morton, on 16th October 1846. He had admistered an ether anaesthetic to enable the chief surgeon at the Massachusett General Hospital to remove a tumour from a patient's neck. Soon afterwards, ether was used by doctors in England and an illustration of the device used was produced in the London Illustrated News on 30th January, 1847, enabling the design to be emulated in the antipodes. With fair winds the best sailing ships could arrive in Austrlaia in 100 days. As a result, announcement of the development appeared in a number of Australian newspapers in May 1847. On 7th June 1847, a Launceston doctor, William Russ Pugh, performed two operations under ether anaesthesia. In the same month Dr John Belisario, a Sydney dentist, and Dr Charles Nathan, a surgeon of Sydney Infirmary, also used ether, this time for dental extractions. |
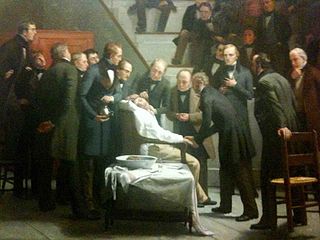
Painting by Robert Hinckley - The First Operation with Ether |
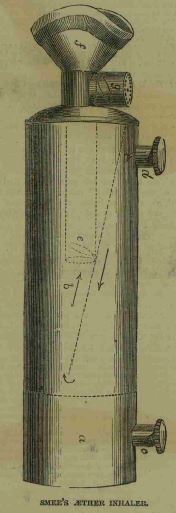
Smee's Aether Inhaler
as illustrated in the London Illustrated News 30th January, 1847.
Courtesy of the British Newspaper Archive |
It is possible, however, that the first use of ether as an anaesthetic in Australia was by Dr Colin Buchanan, a medical officer of the Australian Agricultural Company. At Stroud he used ether to anaesthetise a patient so that he could tie off a popliteal aneurysm. An article in the Sydney Morning Herald, 6th July 1847 (page 3), reproduces the contents of a letter from Buchanan to Captain Phillip Parker-King (Commissioner of the Australian Agricultural Company), in which Buchanan describes the operation and the success of using ether. The letter had been written on the 21st of the month, but the article does not state whether that month was May or June. Of interest, Buchanan did not know how to administer the ether, so made a simple bladder and mouthpiecce. He tried it on himself first!30 |
1847 also saw the first use of chloroform as a general anaesthetic. James Simpson, an obstetrician in Edinburgh, started using it with his patients from this year onwards. A death in 1848, attributed to the use of chloroform, set its usage back.
The use of ether anaesthesia revolutionised surgery as it meant that not only was the patient without pain, but that the doctor could now take his time. No longer was the mark of a surgeon how quickly he could perform an operation but how well he could perform it. Anaesthesia also opened up the possibility of surgery to the abdomen, thorax and head.
The 1850s
Most doctors are now working privately on a fee-for-service basis and
seeing those who could not afford to pay, for free. Some had otherforms
of income eg contracts with the benevolent societies, or capitation fees
for registered patients.
In 1852 some of the PPMA members helped form the Victoria Medical
Association (VMA).
1850 - There are 284 registered doctors in NSW.
1853 - The Medical-Chirurgical Association of Victoria was formed.
1853 - The Castlemaine Medical Association was established
1854 - Mt Alexander Medical Association
1854 - Bendigo District Medical Association
1855 - The Victoria Medical Association and the Medical-Chirurgical
Association of Victoria were amalgamated to form the Medical Society of
Victoria (MSV)
1855 - The NSW Medical Registration Act required applicants to the Medical Register to have at least three years study.
1856 - The Australian Medical Journal commences and runs until 1914.
1857 - The Sisters of Charity opened St Vincent's Hospital in Sydney
1857 - In England a committee formed to draw up "a nomenclature of
diseases to be used in the military services and in civil life". Members
of the committee were drawn from the College of Physicians, the Society
of Apothecaries, the College of Surgeons, the Registrar General, and
the medical departments of the army, navy and the East India Company.
(?the first standardised medical classification system?)
1858 - The The British Medical Act established a single register for all
medical practitioners and determined the qualifications that were
acceptable and who could work in hospitals. This register extended to
all the British colonies.
1858 - England. The curriculum for the medical studies (the Society of
Apothecaries) included examinations in the following subjects; anatomy,
physiology, chemistry, practical chemistry, botany, materia medica, the
Latin of the Pharmacopoeia, prescription, principles and practice of
medicine, midwifery (including the diseases of women and children),
forensic medicine, toxicology and morbid anatomy6
1859 - The Australian Medical Association is formed in Sydney by Dr William Bland. It lasts until 1869.
The 1860s
1860 - The average mortality rates for Australia peak at 2,059 deaths per 100,000 population per year. This remains the highest ever figure recorded since 1856 when reasonable records were regularly obtained for all states.23
1860s - Perinatal mortality was about 1:10.23
1862 - Melbourne University established the first medical school.
1864 - There are 335 registered medical practitioners in Victoria.
1868 - The Medical Association of Victoria (MAV) was formed. It published The Australian Medical Gazette
At about this time a brach of the British Medical Association (BMA) was
formed in Victoria with about 30 members. This worked together with the
MSV for a while, with the MSV's activities focussing on the science of
medicine and the BMA on meico=political issues and ethics. The two
organisations were plagued with dissent and in-fighting to the point of
resignation of Council.
The 1870s
1874 - The Compulsory Vaccination Act in Victoria is passed. All
children were required to be vaccinated against smallpox by six months
of age.
1874 - The first IV anaesthesia was administered by Ore on 9th February 1874.
1875 - The Australian Health Society began in Melbourne. Its focus was
on public health.
1875 - Sixty medical practitioners petition the NSW Legislative Assembly
for a determination to self-regulate the profession. This entailed:
- the ability to accept or decline membership in order to reject those of infamous conduct
- the ability to deal with imposters
- recognitions of doctors who had achieved their status through significant study
The 1880s
Compulsory notifications of infectios diseases begins.
Immigrants with specialist medical/surgical qualifications arrive in lager numbers.
1881 - There are 454 registered medical practitioners in Victoria (after the gold rush).
1881 - The first NSW Board of Health was established under the Infectious Diseases Supervision Act, because of the smallpox epidemic.
1883 - Sydney University's Medical School begins.
1885 - THe first female medical student in Australia is enrolled at Sydney University.
1885 - Adelaide's medical school begins.
1886 - The first Public Health Act (in NSW). Helped define the duties of the Board of Health.
1886 - England. To become a registered medical practitioner one needed to qulaify in medicine, surgery and midwifery. This could be obtained
through the University of London, the College or Physicians, the College of Surgeons or the Sociaety of Apothecaries of London. Candidates would
qualify in either medicine or surgery6. The curriculum is five years. The exams are as follows:
- Primary part 1 - biology, physics, chemistry,materia medica, pharmacy
- Primary part 2 - anatomy, physiology, histology
- Final -
- Section 1 part 1 - principles and practice of surgery, etc (written and oral)
- Section 1 part 2 - principles and practice of medicine, etc forensic medicine, etc (written and oral)
- Section 1 part 3 - midwifery, gynaecology, etc
- Section 2 part 1 - clinical surgery
- Section 2 part 2 - clinical medicine and medical anatomy
Successful candidates were able to stlye themselves LSA (Licenciate of
the Society of Apothecaries) and would also receive a certificate in
dispensing.
1889 - Doctors are required to have their photographs taken as part of their registration.
 |
This requirement persists until 19275
Dr Walter Wignall's registration photograph, 1892. The reverse is stamped with the NSW Medical Board's stamp and the date.
Picture courtesy of and © State of New South Wales through the State Records Authority of NSW 2016
|
The 1890s
Australia entered into a depression.
Age and invalid pensions were introduced.
1890 - Dr Constance Stone became the first registered woman doctor in Australia.
1892 - There are 691 registered doctors in NSW.
1896 - The Medical Benevolent Fund of New South Wales is formed "to
afford assistance to any duly qualified medical man, widow or orphan
children of such, whom the Committee deem worthy of assistance.". It
continues until 1934.
1896 - The Queen Victoria Memorial Hospital was established by the three
sisters, Drs Constance, Clara and Mary Stone for treating women and
children.
1898 - the first spinal anaesthetic is performed by Dr August Bier.
1899 - The NSW Royal Commission on Public Charities examined the running
of agencies receiving government subsidies. A recommendation was that
all hosptials should be placed under governmenr supervision and work
under licence.
The 1900s
Prior to the twentieth century, hospitals were essentially places for poor people to receive medical treatment. The rich were treated at home where possible. Hospitals were often seen as places to go to die. Consequently people did not often go unless they were near death. In the twentieth century, the increasing sophistication of medicine meant that hospitals became places where specialised treatment, not available at home, could be administered.
1900 - The Medical Practitioners (Amendment) Act 1900 (Act No. 33, 1900) was passed. It imposed penalties on persons using titles including Surgeon or Physician if they were not appropriately registered.
1901 - Caudal anaesthesia is independently described by Drs Jean-Anthanase Sicard and Fernand Cathelin in France.
1901 - Federation commenced.
|
|